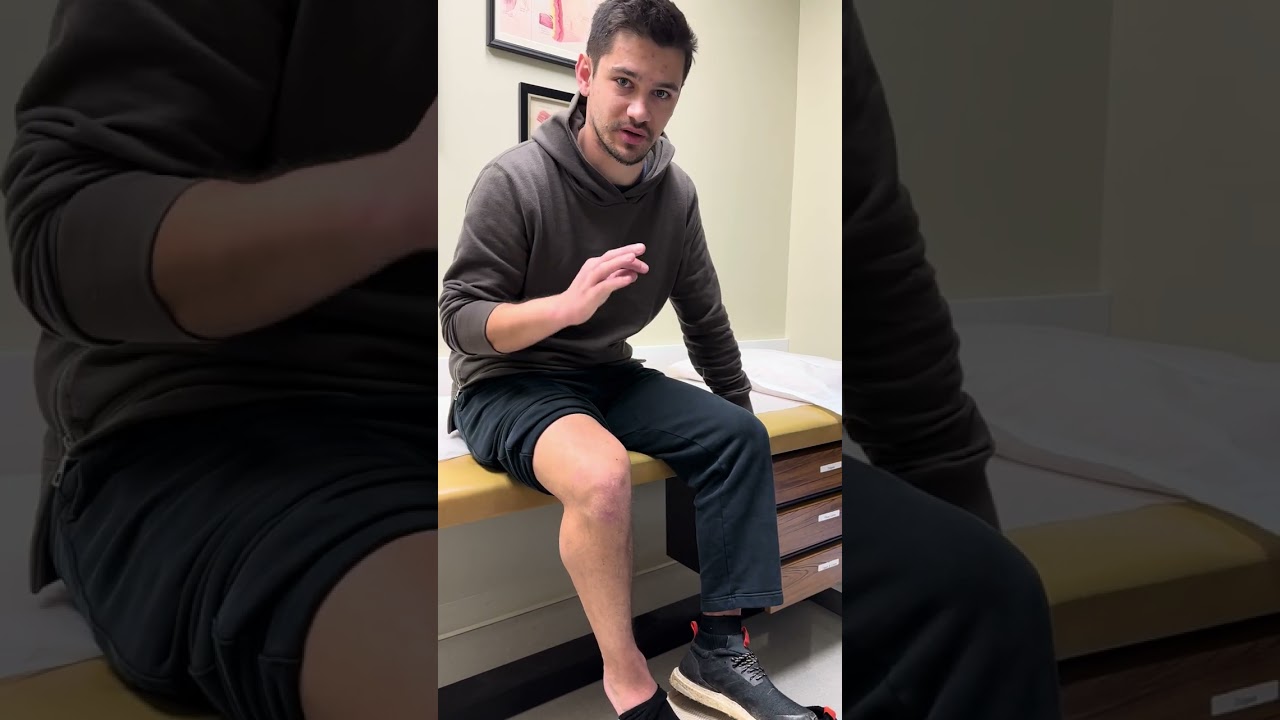
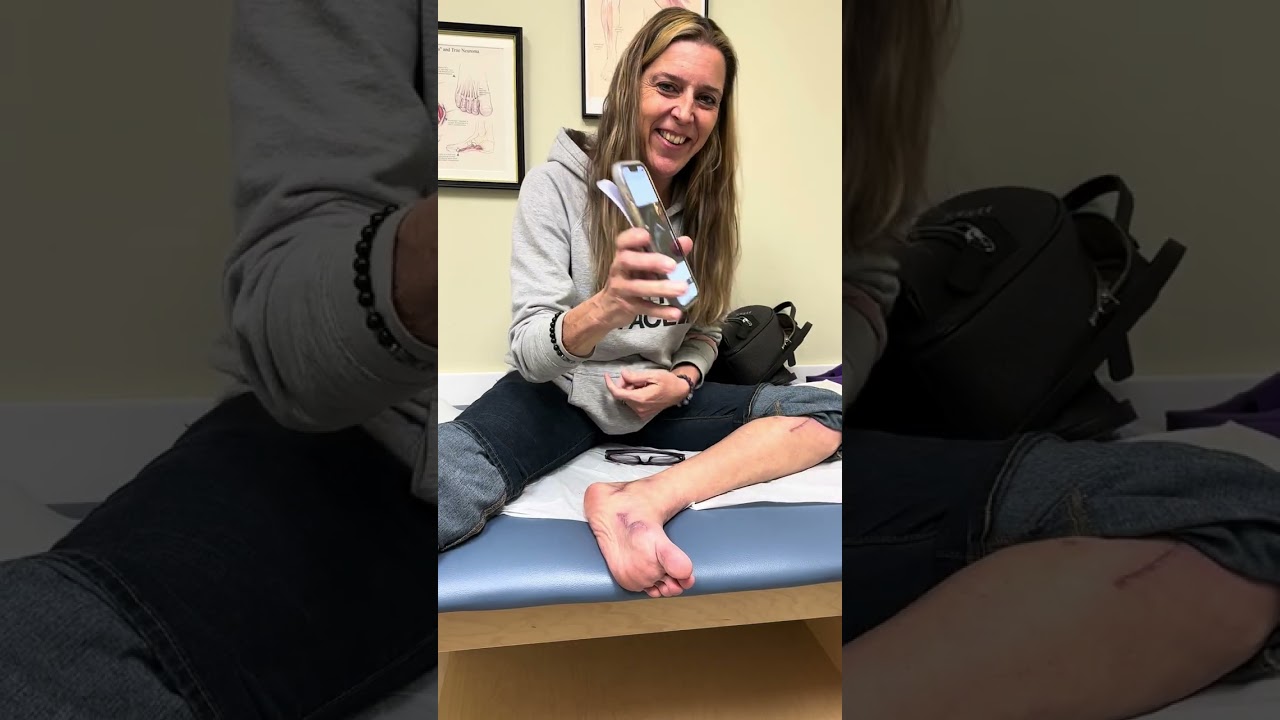
It’s easy to take them for granted, but your lower limbs are marvelously complicated structures. The truth of the matter is, they need to be to perform their important responsibilities of keeping us upright and mobile. This means they’re comprised of numerous bones, muscles, and connective tissues, along with an extensive network of nerves allowing everything to function the way it should.
Of course, this also means there is a lot of opportunity for things to go wrong. When they do, sometimes it can be a challenge to determine what is happening. Dr. Eric H. Williams—a plastic surgeon with specialized training in peripheral nerve surgery—specializes in the diagnosis and treatment nerve related problems in the foot and ankle.
Many nerve compressions or entrapments and injuries can occur in the foot and ankle, creating severe pain and substantial disability. If left untreated, or treated improperly, the symptoms can last for years.
When basic or traditional medical or podiatric care doesn’t improve the symptoms you are experiencing in your foot or ankle, and orthopedic workup does not support a problem with bones, joints, ligaments, or tendons, then pain from peripheral nerve origin is quite probable. If your pain consists of burning, tingling, pins and needles, hypersensitivity, numbness, or sharp, shooting pain, there is a high likelihood your pain neuropathic.
Table of Contents
Types of Ankle and Foot Pain
There are numerous reasons why you may be experiencing pain in your ankle or foot, including:
- Chronic pain after ankle sprain and trauma. Following an ankle sprain, you need to take it easy and allow the injured joint, tendons, and ligaments to heal correctly. Too many people, though, have a “just walk it off” mindset and are quick to jump back into physical activity. This can cause ankle instability and chronic pain in certain cases.
We strongly recommend seeking an evaluation by an appropriately trained foot and ankle specialist if you have severe pain. This also holds true if your pain does not respond to traditional “rest, ice, elevation, and anti-inflammatories” care. The specialist will be able to determine if you have orthopedic injuries—like bone fractures, torn ligaments, ruptured tendons, etc.—that will require more aggressive treatment. As a further consideration, keep in mind you should expect pain following physical trauma to improve over time.
One area of pain frequently passed over and poorly-treated in patients with ankle sprains is pain related to nerve injuries (such as stretch traction injury). The overall medical and surgical communities are quite good at treating problems we are able to see—broken bones, ruptured tendons, blatantly-cut nerves, etc.—but there is either reluctance or lack of training in treating patients who have pain from sources we are unable to see.
Studies can be done to try detecting nerve injuries in the body. The most common of these is the EMG or nerve conduction studies. Whereas these tests are helpful, they do not always tell the whole story. It’s not uncommon for patients to have quite painful nerve injuries despite “normal” results from the tests. A properly-performed physical exam and careful evaluation of sensory or motor function can often help localize common nerve injuries or entrapments in the lower extremities. This is instrumental in leading to successful treatment so the patient can resume normal motor function as soon as possible. Dr. Williams has been using these diagnostic tests and treatment methods since 2006.

If you’ve had pain in a foot or ankle for more than 6 months following either a simple or complex ankle sprain, in spite of appropriate care from a well-trained physician, we may be able to help you. If you can describe your pain as burning, tingling, hypersensitive, “pins and needles,” numbness, or weakness in motor function—even though medical professionals say “we can’t find anything wrong with you”—we may also be able to help. We encourage you to learn more in our report: "Chronic Pain After an Ankle Injury"
Common injuries following an ankle sprain or fracture include stretch traction injuries, tarsal tunnel syndrome, and entrapments of the common, superficial, and deep peroneal nerves. Fortunately, we specialize in this area and will determine if our techniques will be able to help your case.
- Common, superficial, and deep peroneal nerve entrapments. Your sciatic nerve—the largest nerve in your body—runs from the lower spine and down to your foot. This nerve is comprised of two major branches – the common peroneal and the tibial nerves. The common peroneal nerve then splits into the deep and superficial peroneal nerves at the fibular head, the bone on the bottom outside of the knee joint. Due to various causes, these nerves can become entrapped, which then leads to an array of undesirable symptoms.
One potential symptom of a peroneal nerve entrapment is drop foot – a condition wherein the affected nerve leaves you unable to properly pick up the affected foot when you take a step, so instead you drag it along the ground when you walk. Another sign of foot drop may be the muscles on the outside of your lower leg losing function causing, your ankle to roll outward very easily and leading to instability. A patient may lose function of all of these muscle, which causes significant disability.
There are many causes of foot drop. It can occur after an injury to the spine, the sciatic nerve, the common peroneal nerve, or even its branches of the superficial and deep peroneal nerves. It may happen after a severe ankle sprain, total knee or hip replacement, or herniated disk in the back. Patients could have a ganglion cyst or a nerve tumor that can cause a foot drop – if they are in the “wrong place.”
Depending on the type of peroneal nerve entrapment you are experiencing, Dr. Williams has techniques that have been proven to be successful in addressing these problems. If you are suffering from pain or loss of function due to one of these conditions, contact us at our office in Baltimore, MD office for a consultation. Dr. Williams will assess your particular case and determine if any of his techniques for relieving sciatic nerve or peroneal nerve entrapment are right for you. If surgery on the nerves in the leg is not appropriate for you – he will make sure you are referred to the correct team that will be best suited to help you.
It should be kept in mind that “foot drop” is a time-sensitive problem. In this situation “time is muscle.” The faster the problem can be addressed, the better the outcome may be. If you have a foot drop for greater than 6 months – it is absolutely imperative to have it evaluated as quickly as possible to see if there are simple techniques that could improve this for you.
- Tarsal tunnel syndrome (posterior tibial neuralgia). People tend to be more familiar with the carpal tunnel syndrome that may develop in the wrist, which can be attributed to the frequent use of keyboards, repetitive trauma, positioning, and diabetes. Tarsal tunnel syndrome is a similar issue, however, that can develop in your foot and ankle and cause the same kinds of symptoms – tingling and burning nerve pain in the sole of the foot and heel.
In both of these conditions, there are natural “tunnels” that allow the peripheral nerves traveling from your spine into the hand or foot. In the case of tarsal tunnel syndrome, the nerve moves from the spine, down the leg, and then across the ankle joint into the foot. The tibial nerve travels through the tarsal tunnel at the ankle, then splits into three branches called the medial plantar, lateral plantar, and calcaneal nerves. Each one of these three nerves has its own tunnel as well that often needs to be addressed in patients who suffer from tarsal tunnel syndrome.
Dr. Williams specializes in treating patients who have been diagnosed with tarsal tunnel syndrome. While he is an expert in treating patients who have failed previous attempts at tarsal tunnel release, he prefers to be the first one to evaluate, confirm, and treat patients with tarsal tunnel syndrome. Dr. Williams is a disciple of A. Lee Dellon, MD, Ph.D., who has pioneered and championed alterations in the traditional techniques for surgical management of tarsal tunnel syndrome. These revolutionary alterations have greatly increased the success rate of surgery for tarsal tunnel syndrome, while at the same time significantly decreasing complications and improving recovery.
- Morton’s neuroma (digital nerve entrapment). A Morton’s neuroma is more accurately known as an interdigital nerve compression. This means the nerve traveling to the toes is compressed or pinched between the bones on either side. The most common position for this to occur is in the 3rd web space – but these nerve entrapments can occur between any of the toes in the ball of the foot.
Dr. Morton was the first person to describe this long ago. Back then, because there were no effective ways to treat this disease in the early stages, the digital nerve would become so inflamed and so angry that it looked a tumor or a neuroma (which is a ball of nerve tissue that develops when a nerve is cut and tries to regrow.) The treatment of choice used to be to cut these entrapped nerves out. This leads to increased numbness in affected toes, but the tradeoff is hope of getting rid of your pain. While this used to be the gold standard of care and is still practiced by most of the foot and ankle surgeons in the world, there are some problems with this approach.
The main problem is the fact some patients who have these nerves cut out develop a true neuroma – which as mentioned above – is a painful ball of nerve tissue that forms as the nerve tries to regrow. This can actually be a much worse problem than the original “Morton’s neuroma.” In the past 15 years, a transition has been taking place in the medical community which tries to preserve the digital nerves by “decompressing” them instead of cutting the nerves out. This hopefully prevents a painful “true neuroma” or a “stump neuroma” from forming at the cut end of the nerve.
Many podiatrists may be able to relieve early symptoms of Morton’s neuromas with conservative (nonsurgical) care, and if this works, that is preferred. However, when the symptoms do not resolve with conservative care, Dr. Williams performs surgical procedures to relieve the pressure on the nerve – while preserving the nerves – if at all possible. If the nerve is too badly damaged, then sometimes the nerve does need to be removed, but even in this situation, Dr. Williams uses techniques to try and limit the likelihood of a “stump neuroma” developing.
Dr. Williams is an expert in treating patients who have had previous surgery for a Morton’s neuroma but are still experiencing chronic pain (and may even be worse than they were before surgery). He also specializes in treating those who have been newly-diagnosed with Morton’s neuroma and found conservative therapy not to help.
- Post-surgical pain. The reason you underwent surgery was to address a problem. Sometimes, patients still experience pain beyond a reasonable amount of time, which is known as chronic pain. When this happens, Dr. Williams may be able to provide the relief you need. First, he will seek to understand your symptoms and how they may be related to a previous surgical procedure that was supposed to make you feel better, and then determine what may have happened.
Depending on your case, it is possible:
- A nerve was injured during the procedure or stuck in scar tissue
- There was another diagnosis that had been “masked” by the original condition addressed by your prior surgery
- The initial procedure was simply unsuccessful
Some of the more common post-surgical pain issues in the foot or ankle happen following bunion surgery, Morton’s neuroma surgery, tarsal tunnel release, or ankle bone or tendon reconstruction. After determining what may have occurred, Dr. Williams will decide if one of his techniques may be able to help you. At that point, you can decide which direction for treatment you would like to pursue.
- Post-amputation pain or phantom pain. When it comes to amputations in the lower limbs or toes, the two most common sources are physical trauma (car accidents, etc.) and chronic wounds. Most patients expect to be cured of their pain by an amputation, and it can be very disheartening when there is more pain after amputation than before.
Post-amputation pain or phantom pain is not uncommon and can be challenging to treat. Dr. Williams has techniques that have proven successful for other patients by moving nerve endings stuck in scar tissue, injured as a result of the trauma that led to the amputation or injured by the trauma of amputation surgery itself. Of course, every patient is a unique case, so it is important to come in for a consultation.
Treating Ankle and Foot Pain
In most cases, a podiatrist will be able to help you with foot and ankle pain. When your podiatrist or foot and ankle surgeon cannot provide the relief you need, Dr. Williams may be able to create a successful treatment plan for you. He has an array of proven surgical techniques, and can also revise existing procedures if the situation warrants doing so.
Treatment plans are customized for every patient since every case is unique. This means Dr. Williams will take the time to actually listen to you, carefully diagnose the root of the problem, and then work to create your treatment plan. It is important to note that this process relies on you being as honest and candid about the way you are feeling and symptoms you have. Our office provides an environment wherein you can feel safe discussing exactly what is happening, and then we can work on solving it for you.
Contact Dr. Williams Today
For additional information on ankle and foot pain treatment, give us a call at (401) 337-5400. Our friendly staff will be glad to answer any questions you have and help you set up your consultation with Dr. Williams. Your path to pain relief begins with this simple step, so call our Baltimore, MD office today!